In this section : Emergencies
Blunt Chest Wall Trauma/Rib Fractures
Fracture Management Guidelines (Paediatric)
Fracture Management Guidelines (Adult)
Hypothermia
Care Of Burns In Scotland (COBIS) Paediatric Guidance
Paediatric Febrile Neutropenia Guidance
PAEDIATRIC HYPOGLYCAEMIA MANAGEMENT in NON DIABETIC CHILDREN
Management of Anaphylaxis (Paediatrics)
Management of Prolonged Seizures (Convulsive Status Epilepticus) in Children
Acute Wheeze or Asthma in Paediatrics
Medical Emergencies in Eating Disorders (MEED)
Emergency Department
Vasopressors and Inotropes/Chronotropes
Shock
Level 1 CCU Medical Area
Pericardiocentesis
Major Haemorrhage Protocols (DGRI & GCH)
Major Haemorrhage
Suspected Anaphylaxis
Home | Articles | Emergencies |
Suspected Anaphylaxis
Last updated 18th May 2021
Key Points
- Anaphylaxis is a severe, life threatening, systemic reaction that can affect people of all ages. It is caused by release of biologically active chemical mediators from mast cells or basophils.
- It is characterised by rapidly developing, life-threatening problems involving: the airway (pharyngeal or laryngeal oedema) and/or breathing (bronchospasm with tachypnoea) and/or circulation (hypotension and/or tachycardia).
- Other features are often present such as urticarial and angio-oedema of the face.
- IM Adrenaline is the first line treatment for anaphylaxis, reserving IV Adrenaline for cardiorespiratory arrest.
- In emergency departments a person who presents with the signs and symptoms listed above should be classified as having ’suspected anaphylaxis’ rather than an ‘anaphylactic’ reaction until diagnosis confirmed – in 50% cases the label is removed.
Management
- 0.5ml (500micrograms) 1:1000 IM Adrenaline. Best injection site is lateral thigh, using green needle. Repeat after 5 minutes if no clinical improvement
- High flow oxygen
- 10mg Chlorpheniramine IM or slowly IV, with Hydrocortisone 200mg IM or IV
- 1.0 – 1.5 litres 0.9% Saline IV if clinical manifestations of shock dont respond quickly to drug treatment.
- Call 2222 – Adult Resus team in event of cardiorespiratory arrest.
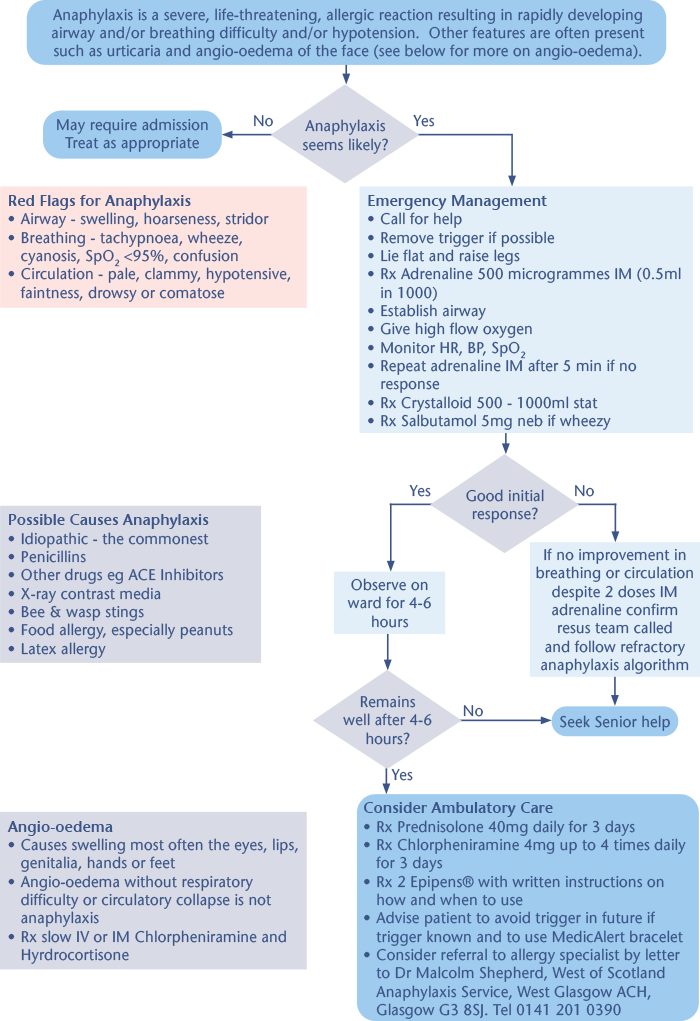
Suspected Anaphylaxis Algorithm
When to Measure Tryptase
- Serum tryptase levels may help diagnose retrospectively
- Send blood in serum gel tubes at <30min, 1 – 3 hrs and 24hrs post event, with special request form that can be downloaded from DGRI laboratory services website.
- Samples go to Gartnavel Hospital with turnaround of 2-4 weeks
- Normal range less than 13 micrograms/L – demonstration of rise and fall is necessary to confirm anaphylaxis
Biphasic Reactions
- Biphasic reactions occur in up to 20% patients, so you should observe all patients who have had an anaphylactic reaction in an appropriate setting with resuscitation facilities for 4-6 hours.
- You can reduce the risk of a biphasic reaction by giving Hydrocortisone with Chlorpheniramine as above, followed by a 3 day course of oral Prednisolone and oral Chlopheniramine
- Prior to discharge the patient should be reviewed by a senior clinician, given clear instructions to return if symptoms return and considered for an adrenaline autoinjector.
Auto-Injector Epipens®
- Prescribe two adrenaline autoinjectors (Epipen®) following anaphylactic reaction, if difficult to avoid the allergen eg nuts.
- Advise patients to use if they have difficulty breathing or become faint. Delaying treatment with adrenaline is associated with longer hospital stays and increased risk of death.
- Teach patients and family how and when to use their autoinjector and make sure they know they should replace them before the expiry date.
- Note autoinjectors have shorter needles and may inject Adrenaline into SC tissue resulting in slower absorption
- Adult dose of Adrenaline in Epipen® is 300micrograms. Advise a second dose five minutes after the first dose if gets worse or fails to improve.
- Always call for an ambulance after using autoinjector even if feeling better because of risk of biphasic reaction
Angio-Oedema
- Angio-oedema is painless oedema affecting the lips, eyelids, genitals, hands, and feet. When affecting the eyelids, the whole socket is usually involved. Angio-oedema involving the upper respiratory tract may result in life threatening airway obstruction.
- This can occur with life-threatening respiratory difficulty or circulatory collapse but does not always do so.
- May be associated with urticaria.
- Consider adverse drug reactions, esp ACEI and NSAIDs, in patients presenting with angio-oedema in the absence of urticaria
- Usually responds to treatment with antihistamines and, in severe cases, steroids.
- C1 esterase inhibitor deficiency is a rare cause of angio-oedema without urticaria. It should be excluded with blood tests (C4 and C1 inhibitor levels), as treatment for this condition is different.
Urticaria
- Urticaria characterised by appearance of wheals
- May occur on its own, accompany angio-oedema or be present in anaphylaxis
- Acute urticaria may be caused by sensitivity to foods or drugs eg antibiotics, NSAIDs, opiates, blood products and radiocontrast media. In 50% the cause is not identified.
- Mainstay of acute urticaria management is avoidance of allergen/cause and treatment with antihistamine
ACE Inhibitors
- Angio-oedema due to angiotensin converting enzyme inhibitors occurs in 0.1% to 1% of patients who take these drugs. Reactions can start at any time, and may occur years after starting the drug.
- Angio-oedema to ACEI is a class effect rather than an idiosyncratic effect and a history of idiopathic angio-oedema or previous ACEI induced angio-oedema is an absolute contraindication to their use.
- Patients developing angio-oedema with ACEI should be ok with ARBs as these drugs have no effect on bradykinin system – studies suggest angio-oedema risk of <10%. Risk of angio-oedema in hypertension is higher with Amlodipine than with ARBs.
- Beta blockers or Calcium channel blockers are safe alternative antihypertensive drugs in patients with ACEI angio-oedema.
Contact Dermatitis
- Contact dermatitis is caused by sensitivity to topical medication, either to the active component or to the preservative. Cosmetics, including nail polish, may also be the cause.
Latex Allergy
- Consider if anaphylaxis occurs during medical or dental procedure
- Patients allergic to latex may also be allergic to bananas, avocados,chestnuts and kiwi fruit because of proteins in these fruits that cross react
Peanut Allergy
- A variety of medications may contain peanut (arachis) oil, including topical creams and emollients, ear wax softening solutions, and enemas.
- Patients with a history of peanut allergy should not use medications containing peanut because of the high risk of a systemic reaction.
Follow Up
- All patients with anaphylaxis (not urticaria) should be referred to West of Scotland Anaphylaxis Service in Glasgow for further elective assessment after they have recovered.
- Referral should be by letter to Dr Malcolm Shepherd, West of Scotland Anaphylaxis Service, West Glasgow Ambulatory Care Hub, Glasgow G3 8SJ. Contact number is 0141 201 0390.